Society for East Asian Anthropology
By Xisai Song
September 16, 2020
This piece is part of an SEAA series on “An Anthropology of Ethics in East Asia.” The articles examine how individuals cope with societal changes such as environmental crises, nationalism, economic development, and mobility through a lens of everyday ethics.
As a life-sustaining treatment for patients suffering from kidney failure, hemodialysis has been ridden with controversies since its emergence. It is a “half-way technology” that can neither cure the disease nor provide a sense of comfort, but jams patients into a long and torturing status between life and death (see for example, Fox and Swazey 2001; Kaufman 2015). The life quality for patients on hemodialysis is extremely low: they have to constantly practice self-discipline in food and water consumption (only one small cup of water a day) and chronically experience a long list of complications such as itchy skin, sleeping problems, and bone diseases. Unless acquiring kidney transplants, patients have to depend on hemodialysis until death.
In 2019, I conducted fieldwork in the hemodialysis ward of a public hospital in Qiushui, a poor, mountainous county in northeastern Sichuan, China. There were 95 patients suffering from kidney failure who regularly visited the ward for a four-hour hemodialysis treatment two to three times a week. The majority of them were from the county’s rural areas, among whom most were former migrant workers. They used to work as laborers such as factory workers, construction workers, and truck drivers in coastal provinces in China, but returned to their hometown to receive hemodialysis treatments. Half of these patients were under 45 and 10 of them were in their twenties. In spite of their young age, only six patients in this ward were waiting to receive a kidney transplant. Why do so many patients choose the arduous hemodialysis treatment instead of kidney transplant? How is their clinical decision making formulated in the social-historical and political context of China today?
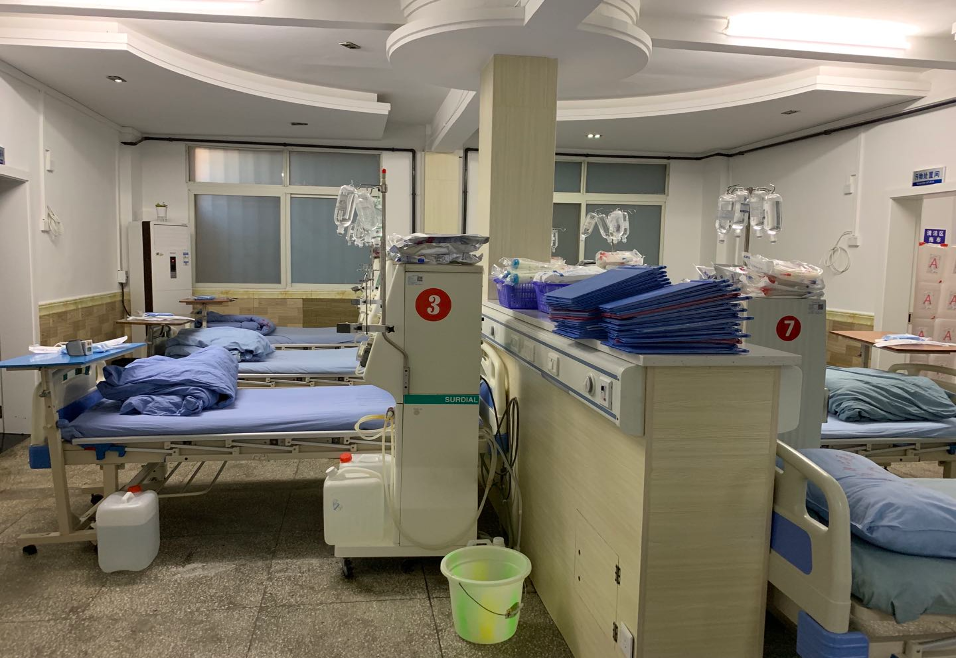
Caption: A corner of the hemodialysis ward. Xisai Song
What shocked me when doing fieldwork in the hemodialysis ward was how grateful those patients were to the state, in sharp contrast to what has been documented in anthropological studies in other contexts where poor patients attributed their reluctance to receive kidney transplants to social and structural problems (for example, Hamdy 2012). Coexistent with their indebtedness to the state was patients’ intensive moral anxiety and self-blame. State-sponsored insurance schemes and the “Targeted Measures in Poverty Alleviation” (jing zhun fu pin) program cover 75 to 90 percent of patients’ medical expenses, making hemodialysis financially accessible. These state welfare programs made patients feel included into the political order. At the same time, although migrant workers are constitutive of creating the new socioeconomic landscape of reform-era China (Zhang 2001), they are displaced from it immediately as they lose their ability to work. Unemployment is common among these former migrant workers on hemodialysis because their bodies can no longer handle the heavy labor required to keep their jobs as blue-collar workers. As a result, families, both as a cultural source of support (Kleinman 1980; Yan 2017) and an agent of the biopolitical state (Ma 2020), become the default safety net that patients depend on for financial support and for care. Caring for a sick family member is a long-standing moral norm in China. In poor rural households, however, caring involves meticulous calculations and moral tensions; families strain to coordinate their limited resources including labor, money, opportunities, and life prospects. Consequently, clinical decision making, discursively framed as a private act of family responsibility, is in fact a dilemma of survival. Deciding on treatment options like kidney transplantation entails moral struggles of evaluating and comparing life values among family members.
For Shan, a patient in her early fifties, kidney transplantation was “meaningless.” Instead, her primary concern was her son’s marriage. Shan was from a rural village in Qiushui. She and her husband were factory workers in southern China. In 2013, Shan was suddenly diagnosed with kidney failure and came back to Qiushui to receive hemodialysis treatments. Shan’s husband also quit his job to take care of her, because Shan suffered from serious complications and couldn’t live by herself. Her son, who was 18 then, dropped out of school immediately and started working as a migrant worker to shoulder the financial responsibility of the family. In the past seven years, Shan and her husband had to rely on her son to pay Shan’s medical bills as well as their living expenditures. “I cried every time I received money from my son. I put too much pressure on him,” Shan once said to me. Shan’s son was 25 and remained single, which was absurd in rural areas where the marriage age was early. In Shan’s village, people called her “bottomless pits of trouble” (wu di dong) and no matchmaker ever introduced a girl to her son. Shan’s son also didn’t find a girlfriend in his workplace. Shan was extremely guilty that her son hadn’t finished school and blamed the difficulty of her son getting married on herself. Shan never considered kidney transplantation, refusing to add more burdens to her son. The financial cost of post-transplant medications was comparable to that of hemodialysis, while the possibilities of recurrent hospitalizations and relapse of kidney failure would further their trouble. Shan’s biggest wish was that her son would build a family of his own before her own death. Her family spent a large portion of their savings remodeling their house in 2019. A new house is an important cultural and economic symbol indicating that a family is ready to welcome a daughter-in-law. Bioethical principles of informed consents and patient autonomy have gained plenty of anthropological scrutiny.
In addition to worries over financial and caring burdens, many young patients regarded kidney transplantation as “useless.” The story of Jinwei, a patient in his mid-thirties, is one example. Growing up in a rural village of Qiushui, Jinwei went to Guangdong, a southern province at the age of 16 in 1998. Jinwei aspired to make a fortune and to snatch a good place in China’s emerging market economy. He started as a factory worker, but later became a gang member. Although his income was much higher, he ended up getting imprisoned for three years. After his release, he went back to working in a factory. Jinwei described the 1990s as a golden age of opportunity. Seeing some of his old friends getting rich, Jinwei was determined not to be left behind. He went to Beijing and invested his life savings into running a restaurant. The business failed a few years later, and Jinwei returned to work in a factory. This was where he met his wife, a fellow worker. In 2018, they got married and his wife became pregnant with twin boys. However, in the same year, Jinwei was diagnosed with chronic kidney disease (CKD). His CKD quickly progressed to the end stage and he started hemodialysis in early 2019. His boys were only three months old. Jinwei firmly refused to sign up for a kidney transplant waiting list. People with kidney transplants should still avoid heavy labor. That is to say, transplantation would not change the fact that Jinwei had lost his ability to work. Reflecting on the past 20 years, Jinwei demonstrated a strong sense of regret and failure, thus having no confidence to build a new life with a disabled body if he were to receive a kidney transplant. Jinwei didn’t bother to undertake the risks of a transplantation surgery, but would rather spend the surgery fees on raising his boys. He was immensely remorseful for his inability to provide his boys with an adequate life. Jinwei strictly practiced self-discipline in everyday life in order to maintain his body in a stable condition and to prolong his life, which extended beyond following medical advice to his moral endeavor to be a good father.
Bioethical principles of informed consents and patient autonomy have gained plenty of anthropological scrutiny. Scholars critique bioethics’ underlying liberalism and science-centric frameworks that overlook the complexity of local moral worlds and obscure structural inequalities (see for example, Kleinman 1995; Mol 2008; Pinto 2014; Rapp 2000). For Shan and Jinwei, their treatment choices are neither autonomous nor orient toward themselves. Instead, they gauge the overall well-being of their families and prioritize the benefits of the ones with relatively better life prospects—their children in both cases. Their seemingly intergenerational moral acts such as the sacrifice of Shan’s son, Shan’s motherly love, and Jinwei’s pursuit of good fathering have, however, obscured these poor patients’ predicaments caused by socioeconomic marginalization. For Shan and Jinwei, the chronic effects after transplantation—including the inability to work, long-term medication, and dependence on care—outweigh the benefits that transplantation can bring. Thus, they deem kidney transplantation worthless. Like Shan and Jinwei, most former migrant workers in the hemodialysis ward of the hospital in Qiushui regard kidney transplantation as being of little help to their life hardships, which challenges biomedical standards of medical efficacy. Instead of applying to individual biological bodies, medical efficacy is unevenly distributed to patients of different social statuses.
Xisai Song is a PhD candidate at Cornell University. Her study examines how lower-class patients struggle with chronic kidney disease in China. Her research interests include chronicity, medical ethics, health inequality, and the ways in which biomedicine is contextualized into non-Western contexts.
Cite as: Song, Xisai. 2020. “Clinical Decision Making in Rural China.” Anthropology News website, September 16, 2020. DOI: 10.14506/AN.1498
Copyright [2020] American Anthropological Association